- Procedure Name:
- Upper Eyelid Surgery Procedure
Upper eyelid surgery is an excess skin removal procedure to alleviate moderate-to-severe ptosis for aesthetics or chronically obstructed vision.
- Procedure Name:
- Asian Eyelid Surgery Procedure
An Asian eyelid surgery, also known as double eyelid surgery, combines microsurgery and the understanding of Asian beauty to create natural results.
- Procedure Name:
- Lower Eyelid Surgery Procedure
Get rid of heavy undereye bags and unflattering dark circles with lower eyelid surgery (lower lid blepharoplasty) by Dr. Lee at L Plastic Surgery.
- Procedure Name:
- Facelift Procedure
Dr. Lee performs full or mini facelifts with precision using microsurgical techniques to reposition the facial skin into a higher place on your face.
- Procedure Name:
- Neck Lift Procedure
With a neck lift, you'll have a rejuvenating surgery to remove loose skin and tighten the muscles of the neck. Some patients also opt for liposuction.
- Procedure Name:
- Rhinoplasty Procedure
Rhinoplasty, also known as cosmetic nose surgery, can address both the aesthetic form and breathing functionality of an obstructed airway in the nose.
- Procedure Name:
- Ear Surgery Procedure
We offer two types of ear surgeries at L Plastic Surgery: otoplasty (ear pinning) or earlobe repair to amend congenital deformities or earlobe tears.
- Procedure Name:
- Buccal Fat Removal Procedure
Face fat removal is a surgical procedure offered for patients who have excessive cheek fat that is disproportionate to the rest of the facial profile.
- Procedure Name:
- Facial Fat Grafting Procedure
Naturally rejuvenate key areas of your facial features with facial fat grafts for age-related volume loss and wrinkles with your own harvested fat.
- Procedure Name:
- Breast Augmentation Procedure
Dr. Lee has a variety of breast augmentation options with breast implants or autologous tissue flaps to create an aesthetically pleasing bustline.
- Procedure Name:
- Breast Lift Procedure
A breast lift at L Plastic Surgery reduces the excess skin that has lost its elasticity and elevates the nipple/areola complex into a higher position.
- Procedure Name:
- Tummy Tuck Procedure
Living with unwanted excess skin on your midsection? Consider having a tummy tuck (abdominoplasty) to tighten up the skin and muscles in your abdomen.
- Procedure Name:
- Varicose Veins Procedure
Dr. Lee can provide you with diagnostic ultrasounds and effective therapeutic options for varicose veins, which may include laser vein treatments.
- Procedure Name:
- Liposuction Procedure
Liposuction is an excellent cosmetic procedure to remove fat for men and women with stubborn body fat (even when diet and exercise are on point).
- Procedure Name:
- Breast Reconstruction Procedure
We offer breast cancer survivors and women with a recent breast cancer diagnosis reconstructive breast surgeries by Dr. Lee in San Francisco, CA.
- Procedure Name:
- Phalloplasty Procedure
Dr. Lee performs reconstructive phalloplasty for gender affirmation surgery using the radial forearm flap or ALT flap with the Crane Center.
- Procedure Name:
- Hand and Nerve Surgery Procedure
Dr. Lee is an experienced hand and nerve microsurgeon who has treated prominent Bay Area athletes, musicians, artists, mechanics, and professionals.
- Procedure Name:
- BOTOX® Procedure
Ask about our BOTOX injections if you would like to learn more about wrinkle reduction around the forehead, eyebrows, and Crow's feet without surgery.
- Procedure Name:
- JUVÉDERM Procedure
Give your facial features, such as gaunt cheeks or shapeless lips, more volume with JUVÉDERM dermal filler injections for full facial rejuvenation.
- Procedure Name:
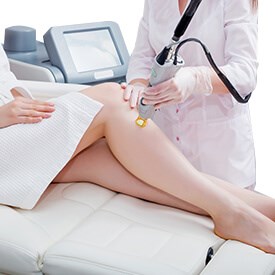
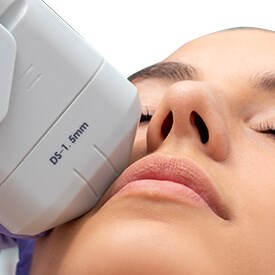
- Laser and Ultherapy Treatments Procedure
Thinking about having a laser or nonsurgical treatment? We offer Spectra, Clarity, and Ultherapy laser sessions at L Plastic Surgery in San Francisco.